Athens Radiology Associates offer the full complement of state-of-the-art breast imaging services. We have six subspecialized breast imaging physicians and a team of nurses, technologists, and sonographers all with a passion for excellent and compassionate care.
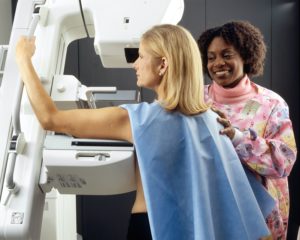
Screening Mammogram
The goal of breast cancer screening is to reduce deaths due to breast cancer by detecting cancer at an early stage when treatment is more effective. For most women, yearly mammograms should begin at age 40. Most women who are diagnosed with breast cancer do not have a family history, and 1 in 8 women will be diagnosed with breast cancer in their lifetime. Multiple studies have shown that annual screening mammograms starting at age 40 saves the most lives. See below to learn more about breast cancer screening and how we evaluate breast cancer risk.


Diagnostic Mammogram
A diagnostic mammogram is performed for women who are having breast symptoms such as a lump, focal pain, nipple discharge, or skin changes. It is also performed for women who have had an abnormality detected on their screening mammogram. A diagnostic mammogram involves additional dedicated views to closely examine an area of interest in the breast. A breast imaging radiologist will review your images right after they are taken to determine whether additional images or a breast ultrasound is needed. You will be given your results by the end of your appointment.
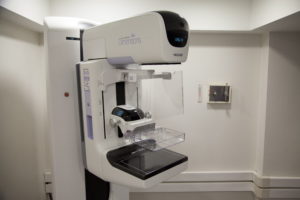
3D-Mammography (Digital Breast Tomosynthesis)
Digital breast tomosynthesis (tomo), also known as 3D mammography, is a screening and diagnostic breast imaging tool to improve the early detection of breast cancer. During the 3D part of the exam, an x-ray arm sweeps over the breast, taking multiple images in seconds that can then be viewed by our radiologists. 3D mammography increases cancer detection rate and decreases callback rates from screening and is particularly helpful to evaluate mammograms for women with dense breast tissue. See below to learn more about 3D mammography and breast density.
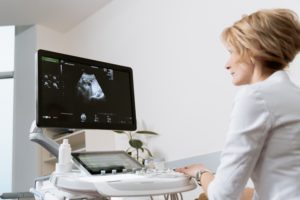
Breast Ultrasound
Ultrasound is a noninvasive medical test that uses sound waves to produce pictures of the internal structures of the body. A breast ultrasound may be performed as part of your diagnostic exam. You will be scanned by a sonographer as well as by a specialized breast imaging radiologist. The radiologist will go over the results and recommendations with you at the end of your exam.
Breast MRI
Magnetic resonance imaging (MRI) is a noninvasive medical test that uses a powerful magnetic field without radiation to produce pictures of the body which are then examined on a computer monitor. ARA’s highly trained imaging specialists use state of the art equipment and software to produce and interpret breast MRI images.


Image-Guided Breast Biopsy
Lumps or abnormalities in the breast are often detected by physical examination, mammography, or other imaging studies. However, it is not always possible to tell from these imaging tests whether a lump is benign or cancer. A core needle breast biopsy is performed by a highly trained radiologist to remove some cells through a hollow needle from a suspicious area in the breast and examine them under a microscope to determine a diagnosis.
Breast Needle Localizations
For women who need breast surgery to remove a cancer or atypical lesion, we can perform an image guided localization to help the surgeon know exactly which area to take out. Ultrasound or mammography is used as a guide to put a wire or radiofrequency reflector through the abnormality in the breast. During the surgery, the surgeon uses the wire or reflector to locate and remove the abnormality. Since most breast cancers we diagnose by mammography are too small to feel, performing an image guided localization helps the surgeon remove the entire abnormal area while conserving as much normal breast tissue as possible.
Ultrasound Guided Cyst Aspiration
Breast cysts are benign sacs of water that form in the breast. They are very common and do not cause a problem for the majority of women. For some women, a cyst may become large and painful. In these situations, we can drain the fluid from the cyst using a small needle under ultrasound guidance.
Consultations for review of outside exams
ARA’s radiologists can review studies you have had done elsewhere and give a second opinion.

